How accurate are Lyme disease tests?
Medically reviewed by Neka Miller, PhD on August 11, 2020. To give you technically accurate, evidence-based information, content published on the Everlywell blog is reviewed by credentialed professionals with expertise in medical and bioscience fields.
Table of contents
- When is a Lyme disease test most accurate?
- Lyme disease testing: how it works
- How do false negatives occur?
- Symptoms of Lyme disease
- Treatment for Lyme disease
- Risk factors and prevention
- Everlywell at-home test for Lyme disease
- Related content
Interested in getting tested for Lyme disease and want to learn more about the testing process? Here, we’ll cover several aspects of Lyme disease testing, including accuracy in the context of false negatives, different test types, and more—so continue reading.
When is a Lyme disease test most accurate?
Lyme disease test accuracy depends on the kind of test under consideration. In general, most Lyme disease tests are designed to detect specific antibodies (in a sample of blood) that the body makes in response to a Lyme infection. But it takes several weeks for these antibodies to build up in the bloodstream, and a Lyme disease test will typically be most accurate once these antibodies have developed.
Lyme disease testing: how it works
Two common lab tests for Lyme disease are the enzyme immunoassay (EIA) test and the Western blot test. These tests measure the antibodies that form when someone is infected with Borrelia burgdorferi (the bacterium that causes Lyme).
Enzyme immunoassay (EIA) test
The EIA test (also known as an ELISA test, which stands for enzyme-linked immunoassay) is what’s typically used to screen for Lyme disease by detecting antibodies for B. burgdorferi.
According to the Centers for Disease Control and Prevention, if the EIA test shows negative for the antibodies, no further testing is needed. However, if this screening test comes back with results that are positive or unclear, a second round of testing—using the Western blot method—is recommended. This second test is referred to as a confirmatory test.
Western blot test
When the EIA test is positive, the Western blot test is usually done next. This two-step (or two-tiered) approach to Lyme disease testing helps reduce the number of false positives. The Western blot test detects antibodies for several proteins belonging to Lyme bacteria.
Other tests for Lyme disease
PCR (polymerase chain reaction) tests detect the DNA of the Lyme bacteria. These tests may be used to aid in the diagnosis of Lyme disease, but should not be considered diagnostic by themselves. The results of PCR tests should be used in combination with serologic tests (tests that detect antibodies) and the clinical symptoms a person presents with.
Testing for co-infections
The Global Lyme Alliance also suggests considering testing for co-infections, like Babesia, Ehrlichia, and Bartonella. Because an increasing number of ticks carry and transmit more than one infection, the tests and treatments for some “co-infections” can be different than those for Lyme disease.
How do false negatives occur?
When it comes to Lyme disease test accuracy, some people wonder why false negatives occasionally occur. (In infectious disease testing, a “false negative” means that the test result says you don’t have an infection when you actually do.)
One key reason why is that both the EIA and Western blot tests are indirect tests. They measure the antibody response to the infection rather than directly checking for the genetic material of the bacteria. It can take several weeks for your body to produce enough antibodies for the tests to recognize them, which can sometimes yield false negative results if the tests are taken too soon after getting bitten by an infected tick.
Symptoms of Lyme disease
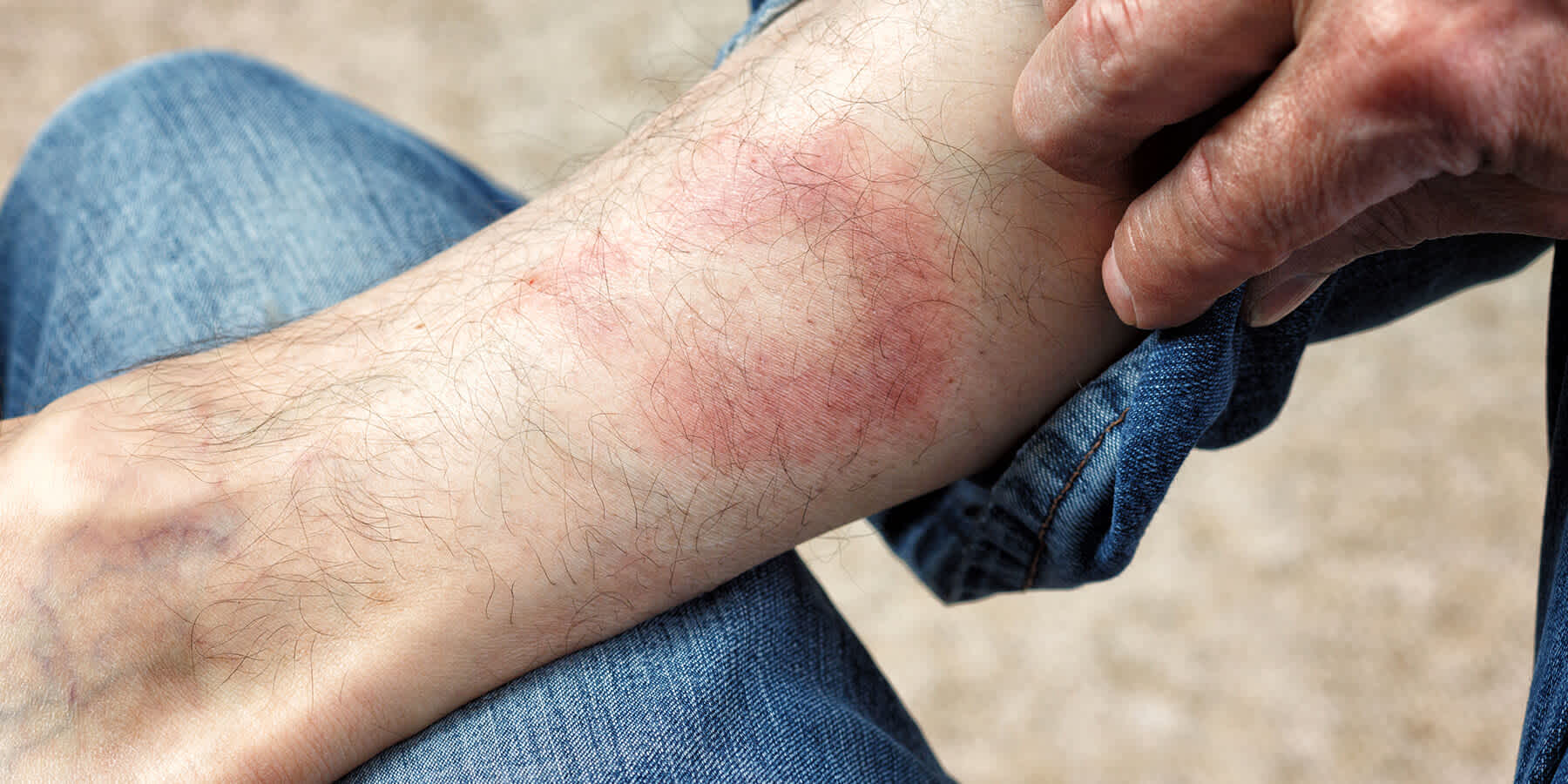
Lyme disease can come with various symptoms. Most notable of these is the characteristic erythema migrans or bulls-eye rash, which occurs in about 70% of infected people. This often begins as a red area near the tick bite. As it expands in size, it often clears in the middle and develops a red ring (or bull’s eye).
Although the rash is a hallmark symptom of Lyme disease, it may look different from person to person. It’s usually not painful or itchy and tends to appear on the thighs, groin, trunk, and armpit.
In addition to erythema migrans, people who are infected with Lyme disease may also experience:
- Fever
- Chills
- Body aches
- Neck stiffness
- Swollen lymph nodes
- Fatigue, including severe fatigue later on during the infection
- Weakness or numbness in arms or legs
- Joint pain which may come and go suddenly and move from one joint to another
- Vision changes
- Heart palpitations
- Chest pain
- Facial paralysis
- Arthritis
- Vertigo
- Headaches
- Sleep disturbance
- Mental confusion
Less common signs and symptoms of this infectious disease include heart problems, such as an irregular heartbeat; eye inflammation; and liver inflammation (hepatitis). These symptoms can occur several weeks after infection.
Later signs and symptoms can include bouts of severe joint pain and swelling. This is common in the knees, though it can also move from one joint to another. Neurological problems can also occur in the weeks, months, or potentially years after infection. You may develop inflammation of the membranes surrounding your brain, known as meningitis, or temporary paralysis of one side of your face, known as Bell’s palsy. Numbness or weakness of your limbs and impaired muscle movement might also be noticeable.
Treatment for Lyme disease
Treatment for Lyme disease requires antibiotics and—in general—recovery is quicker the sooner the treatment begins.
Oral antibiotics
Oral antibiotics are the standard treatment option for early Lyme disease.
Intravenous antibiotics
If this infectious disease affects your central nervous system, your healthcare provider may suggest treatment with an intravenous antibiotic.
Risk factors and prevention
Knowing risk factors and preventative methods for tick bites can help keep you safe. In the United States, deer ticks are mostly found in the heavily wooded areas of the Northeast and Midwest. (Related: What are the chances of Lyme disease after a tick bite?)
Ticks attach easily to bare flesh, so you can protect yourself by strategically choosing what clothes to wear. If you’re going to be in areas where ticks thrive, like wooded areas or areas with tall beach grass, wear a long sleeve shirt and long pants tucked into long socks. Wear close-toed shoes, a hat, and gloves.
When you come in after being outdoors, remove any ticks as soon as possible. A good rule of thumb is to take your clothes off and place them in a hot dryer for 10-15 minutes, as this kills the live ticks. Inspect all areas of your skin and your pet's fur to ensure that no ticks are hiding.
In general, Lyme bacteria from an infected tick will enter the bloodstream if the tick is attached to the skin for 36 to 48 hours—so the earlier you can spot any ticks on you, the better.
Everlywell at-home test for Lyme disease
If you think you’ve been exposed to an infected tick and are suffering from the symptoms mentioned above, our at-home Lyme Disease Test can help tell you if you are positive for a Lyme infection from the convenience of your own home. This test includes both the EIA (screening) and Western blot (confirmatory) assays.
Our test measures IgM and IgG antibody reactivity to three kinds of Lyme disease bacteria: Borrelia garinii, Borrelia afzelii, and Borrelia burgdorferi. The test only requires a small sample of blood, collected with a simple finger prick.
How it works
- Once you order a test, the materials are conveniently delivered to your doorstep.
- You’ll enter the unique kit ID included with your kit at everlywell.com.
- Next, complete a simple finger prick collection and return with prepaid shipping.
- Then, an independent board-certified physician will review your results.
- Once verified, you’ll receive your results on our secure platform within days.
Related content
What ticks carry Lyme disease?
Can you get Lyme disease twice?
What are the chances of Lyme disease after a tick bite?
References
1. Laboratory Diagnostic Testing for Borrelia burgdorferi Infection. Centers for Disease Control and Prevention. URL. Accessed August 11, 2020.
2. Lyme disease. Mayo Clinic. URL. Accessed August 11, 2020.
3. Lyme disease - diagnosis and treatment. Mayo Clinic. URL. Accessed August 11, 2020.
4. Preventing Tick Bites on People. Centers for Disease Control and Prevention. URL. Accessed August 11, 2020.